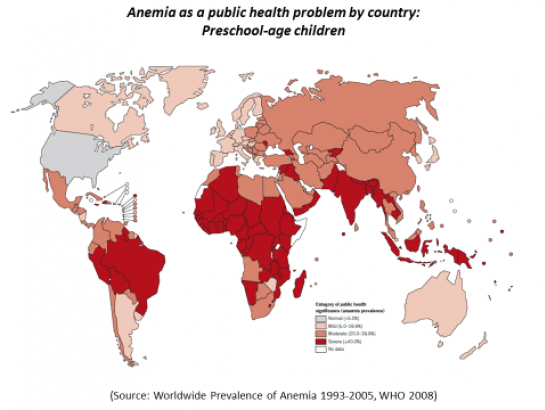
New findings1 from a HarvestPlus-commissioned review challenge the prevailing assumption that 50 percent of anemia is attributable to iron deficiency. The systematic review of 23 countries found that iron deficiency accounts for 25 percent of anemia in young children and 37 percent of anemia in women of reproductive age. Moreover, significant variations exist between countries, which may render generalized assumptions misleading.
How should these findings be interpreted? Should they be acted upon? We asked nutrition experts for their viewpoints, summarized below.
Join the dialogue. We invite you to email your views on these and other related findings to [email protected] and we will post them here.
What major conclusions can be drawn from this paper?
Dr. Tim Green, South Australian Health and Medical Research Institute & Dr. Crystal Karakochuk, University of British Columbia:
- Many factors other than iron deficiency are likely contributing to the high prevalence of anemia.
- It’s important to assess the cause of anemia in each country-specific setting and population.
- Understanding the true etiology of anemia is paramount for the design and implementation of effective anemia reduction strategies and programs.
Dr. Omar Dary, United States Agency for International Development (USAID):
- The data is now clearer that iron deficiency could explain less than half of anemia for developing countries and some middle-income countries.
- The estimation that 25% and 37% of anemia is attributable to iron deficiency in children and women, respectively, coincides with a meta-analysis… which found only 27% of anemia in women could be prevented through intermittent iron supplementation2.
- For children younger than 12, although a 49% reduction of anemia prevalence was reported for the same treatment, variation among studies was very large3, which only shows that the 50% anemia attributable to ID was not more than a very coarse average.
Dr. Reina Engle-Stone, University of California, Davis:
- The specific estimates of proportion of anemia associated with iron deficiency should be interpreted with caution, because 1) the surveys were not representative globally, and the meta-analysis technique combines data from countries that may be very different, 2) there is currently no consensus on adjustment and interpretation of iron biomarkers in the presence of inflammation, which affects the estimated prevalence of iron deficiency and iron deficiency anemia, and 3) cross-sectional surveys permit estimation of the proportion of anemia associated with iron deficiency, but this may not reflect the proportion of anemia that would be resolved by iron interventions.
Dr. Sorrel Namaste, SPRING:
- The findings of this study require us to question our current thinking that 50 percent of anemia is caused by iron deficiency. However, I urge that we proceed with caution.
- The confounding relationship between iron biomarkers (ferritin) and inflammation may result in a substantial underestimation of iron deficiency. And although it was promising that the authors of this paper attempted to address this relationship by applying the categorical Thurnham Correction Factor approach, recent findingsseem to indicate the use of a continuous adjustment approach. Such an approach results in a much higher estimate of iron deficiency4.
What do these findings mean for national anemia reduction programs?
Dr. Green & Dr. Karakochuk:
- National surveys should measure iron deficiency and iron deficiency anemia prevalence, and where possible, this should include a genetic and biochemical assessment of indicators related to inflammation, infection, and iron status.
- The sole measurement of hemoglobin simply does not suffice.
Dr. Dary:
- It may no longer be valid to introduce iron supplementation as the primary intervention for anemia.
- The very common practice of referring to any anemia as iron deficiency anemia must be abandoned.
- Countries must determine the causes of anemia and if iron deficiency is important. If so, interventions to raise the intake of bioavailable iron are important regardless of the contribution of ID to anemia. ID is in itself an important deficiency to correct.
Dr. Engle-Stone:
- A single strategy may not be effective (or cost-effective) for all countries (or, potentially, all regions within a country)
- Programs may need to address multiple causes of anemia, including both nutritional deficiencies and infectious disease.
- It is important to understand the risk factors for anemia in a given population and ensure that this information is used in program design. Program effectiveness should also be measured to adjust the program as needed
Dr. Namaste:
- Interventions to reduce anemia need to match the underlying causes of anemia in a given context.
- Given the existing evidence on iron deficiency anemia's impact on poor health outcomes, I believe we need to ensure we are accurately estimating the problem before dismantling iron interventions.
- It is also important to ensure we are not providing iron to those who do not need it, especially considering safety issues related to administrating iron in settings with a high prevalence of malaria or other infections.
- This all leads back to the importance of assessing the problem. We need to seriously consider what is causing anemia when designing anemia interventions.
What’s next?
Dr. Green & Dr. Karakochuk:
- Assessment of genetic hemoglobin disorders is critical to understand the potential causes of anemia in a population.
- In Cambodia, for example, some hemoglobin disorders have also been shown to be associated with high ferritin concentrations5,6. Naturally existing iron in groundwater may also be a contributing factor to high iron stores with evidence from Bangladesh and Cambodia7,8.
Dr. Dary:
- Iron deficiency must be identified with biochemical tools in a reliable, efficient, and low-cost manner.
- It is essential to determine the normal values for iron-status indicators for children under 2 years.
Dr. Engle-Stone:
- Research is needed to review cutoffs for hemoglobin and iron status indicators with respect to functional outcomes, and the role of adjustment for inflammation in nutrient status assessment; to understand the relative contributions of nutrients other than iron, as well as non-nutritional risks factors for anemia; and to compare the cost-effectiveness of different strategies to address both iron deficiency and anemia.
Dr. Namaste:
- We need to work toward better assessing anemia and the causes of anemia. Stay tuned for the Biomarkers Reflecting Inflammation and Nutritional Determinants of Anemia (BRINDA) results, which will be published soon and will examine approaches to better estimate the prevalence of iron deficiency across countries.
- Iron interventions will likely remain important to anemia reduction efforts, but other factors—such as infections, inflammation, and genetics—may be equally, if not more, important in some settings. SPRING has developed tools to help countries assess their anemia situation at the national and district level9.
1 Petry, Nicolai, et al. "The Proportion of Anemia Associated with Iron Deficiency in Low, Medium, and High Human Development Index Countries: A Systematic Analysis of National Surveys." Nutrients 8.11 (2016): 693.
2 Fernández‐Gaxiola, Ana C., and Luz Maria De‐Regil. "Intermittent iron supplementation for reducing anaemia and its associated impairments in menstruating women." The Cochrane Library(2011).
3 De‐Regil, Luz Maria, et al. "Intermittent iron supplementation for improving nutrition and development in children under 12 years of age." The Cochrane Library (2011).
4 Chichon, Bernardette, et al. "Assessment of Regression Models for Adjustment of Iron Status Biomarkers for Inflammation in Children with Moderate Acute Malnutrition in Burkina Faso." The Journal of nutrition 147.1 (2016): 125-132.
5 George, Joby, et al. "Genetic hemoglobin disorders, infection, and deficiencies of iron and vitamin A determine anemia in young Cambodian children." The Journal of nutrition 142.4 (2012): 781-787.
6 Karakochuk, Crystal D., et al. "The Homozygous Hemoglobin EE Genotype and Chronic Inflammation Are Associated with High Serum Ferritin and Soluble Transferrin Receptor Concentrations among Women in Rural Cambodia." The Journal of nutrition 145.12 (2015): 2765-2773.
7 Merrill, Rebecca D., et al. "High prevalence of anemia with lack of iron deficiency among women in rural Bangladesh: a role for thalassemia and iron in groundwater." Asia Pacific journal of clinical nutrition 21.3 (2012): 416.
8 Karakochuk, Crystal D., et al. "Elevated levels of iron in groundwater in Prey Veng province in Cambodia: a possible factor contributing to high iron stores in women." Journal of water and health13.2 (2015): 575-586.
9 SPRING. "National and District Tools to Guide Anemia Programming." https://www.spring-nutrition.org/publications/series/national-and-district-tools-guide-anemia-programming